
Fetal and Neonatal Neuroimaging: The Role of Imaging in Early Brain Development
Fetal and neonatal neuroimaging has provided a more precise understanding of human brain development from its earliest stages. Through tools such as ultrasound and Magnetic Resonance Imaging (MRI), it is possible to identify structural alterations even before birth.
In the context of congenital infections like the Zika virus, these technologies have been essential for detecting brain damage, understanding its evolution, and improving clinical decision-making during pregnancy and after birth.
The expertise gathered at centers like Sabbag Radiólogos through prospective cohort monitoring has shown that integrating multiple imaging modalities is the gold standard for assessing neurological integrity in at-risk populations.
Prenatal Assessment of the Fetal Brain
During pregnancy, ultrasound is the primary tool for evaluating brain development, allowing for the monitoring of skull growth, identification of structural anomalies, and serial fetal follow-up.
However, fetal MRI has established itself as a crucial complementary technique. In studies led by researchers associated with Sabbag, fetal MRI identified complex anomalies such as nodular heterotopias and cortical development malformations that are not always visible on conventional ultrasound.
MRI provides superior resolution for assessing parenchymal organization and neuronal migration, enabling the detection of lesions even in fetuses with normal head circumferences.
The combination of both techniques enhances diagnostic capability, allowing for a detailed characterization of the severity of brain damage prior to delivery.
This integrated approach is especially relevant in Zika infections, where brain injury has been observed to progress silently during the second and third trimesters.
Neonatal Neuroimaging and Postnatal Follow-up
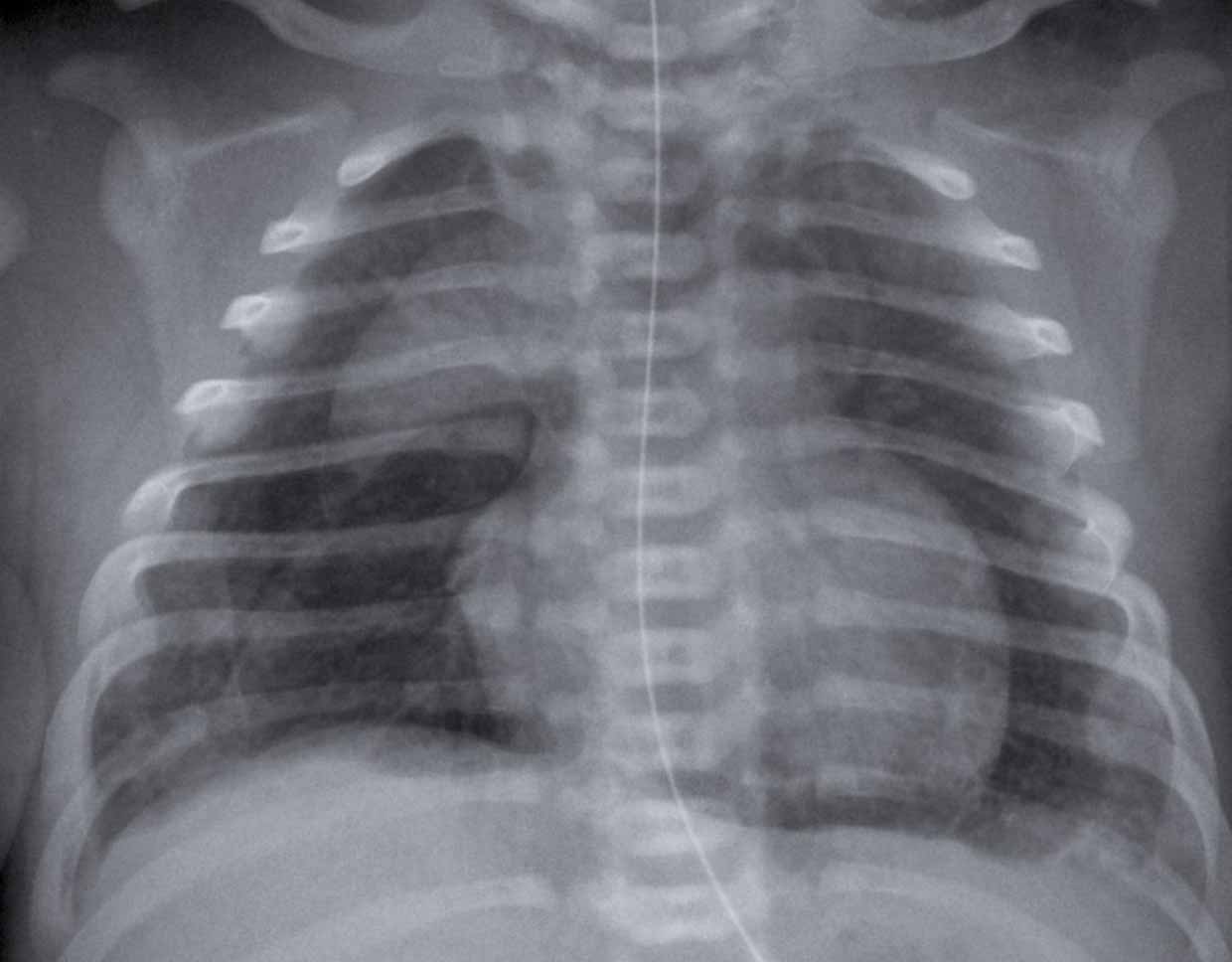
After birth, neonatal neuroimaging allows for the evaluation of the brain under more stable conditions, identifying findings that may not have been detected prenatally due to the technical limitations of the intrauterine environment.
Postnatal cranial ultrasound has shown high sensitivity in detecting subtle findings. In the Barranquilla cohort, this method detected abnormalities in 37% of newborns, including subependymal cysts and lenticulostriate vasculopathy.
Furthermore, neonatal MRI allows for the confirmation of ischemic lesions, calcifications, and myelination delays that are critical for long-term prognosis.
Notably, some newborns with normal prenatal imaging may manifest postnatal findings, reinforcing the need for standardized imaging follow-up protocols.
Longitudinal follow-up is key to correlating these images with neurodevelopment, enabling early intervention for children at risk of motor or cognitive delays.
Clinical Importance and Comprehensive Diagnosis
Integrating different imaging modalities allows for a more complete view of brain development, facilitating more precise and personalized diagnoses.
In Sabbag’s clinical practice, it has been evidenced that brain damage from neurotropic viruses can be evolutionary, requiring a dynamic interpretation of imaging studies.
Neuroimaging serves not only a diagnostic role but also a prognostic one; for instance, detecting reduced brain volumes in normocephalic children is an early predictor of functional alterations.
The interpretation of these studies requires a high level of specialization and close interdisciplinary work between pediatric radiologists, neurologists, and fetal medicine specialists.
This ensures that technical findings are translated into effective clinical management plans for families and healthcare systems.
Innovation and Access in Pediatric Neuroimaging
One of the most significant advances in the collaboration between Sabbag and Children's National Hospital has been the implementation of non-sedated MRI protocols for school-aged children.
By using pedagogical tools such as play tunnels (low-cost simulators) and educational booklets, an 89% success rate was achieved in obtaining high-quality images from 7-year-old children in the Atlántico department.
These strategies significantly reduce risks associated with anesthesia, lower operational costs, and remove logistical barriers for families in resource-limited settings.
Innovation in this field demonstrates that it is possible to conduct patient-centered, cutting-edge research by adapting high-complexity technology to local realities.
This 'mock scanner training' model contributes to strengthening equity in access to advanced diagnostics and improves the quality of data in global neurodevelopmental studies.
Conclusion
Fetal and neonatal neuroimaging has transformed the understanding of early brain development, allowing for the detection of critical alterations before and after birth with unprecedented precision.
The synergy between ultrasound, MRI, and the clinical innovation protocols developed at Sabbag optimizes pediatric care, ensuring that every imaging finding becomes an opportunity for the child's well-being.